About this time every year, the American Association of Endodontists tells us that it’s “Root Canal Awareness Week” – an opportunity for concentrated spin on the wonders of a procedure that’s not all that different from mummification, only with a tooth instead of a complete corpse.
And that’s what a root canal is: a dead tooth. The procedure itself involves scraping out all the living tissue within the pulpal core, leaving merely the shell of dentin and outer enamel. It’s a misguided effort to “save” a tooth that’s beyond saving due to deep decay.
Here’s what it looks like (though if you’re squeamish, you might want to skip it):
Once the pulp has been removed, the dentist does what he or she can to disinfect the hollowed out tooth. And this is where the second set of troubles begin, thanks to the particulars of tooth anatomy, most particularly, the dentinal tubules.
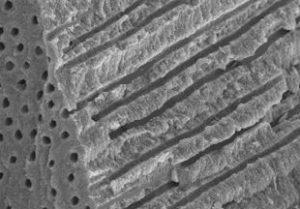 Now, if you’re a regular reader of this blog, you might remember something about these structures. The flow of fluid through them helps your teeth naturally resist decay. But bacteria and other microbes can flow through them, as well – as from an infected pulp.
Now, if you’re a regular reader of this blog, you might remember something about these structures. The flow of fluid through them helps your teeth naturally resist decay. But bacteria and other microbes can flow through them, as well – as from an infected pulp.
But these tubules are microscopic – so small that you find about 3 miles of them in a single tooth. This makes them impossible to clean manually. Only ozone is able to thoroughly penetrate and disinfect these inaccessible tissues – but even then, its effects are only short term once the tooth is filled or crowned.
Once the tooth is sealed at the top, any remaining pathogens are locked within, free to proliferate. And proliferate they do, generating highly toxic byproducts. After all, dark, moist, low-oxygen environments are what oral pathogens like best. The shell of a root canal tooth is thus a perfect environment for them to thrive in.
Though the tooth is sealed at the top, it remains connected to the blood supply at the root.
New pathogens are free to enter the tooth – and, crucially, those in the tooth can escape and enter the bloodstream. Free to travel, they wreak havoc wherever they find opportunity. Here’s where we find the relationship between root canal teeth and a host of systemic health issues, including
- Autoimmune diseases.
- Musculoskeletal diseases.
- Irritable bowel diseases such as Crohn’s.
- Fibromyalgia.
- Depression.
- Cancer.
Cancer expert Dr. Josef Issels found that nearly all patients visiting his groundbreaking cancer clinic – 98% – had infection stemming from supposedly sterile root canal teeth. Toxicology expert Dr. Boyd Haley has found that about 90% of root canal teeth are teeming with dozens of different pathogens.
 Now, this doesn’t mean that if you have root canals, you’re fated for cancer or other chronic disease. As we’ve noted before, the development of illness – and the type of illness that manifests – depends upon the health of your biological terrain. Just as there are some who can live for years with mercury fillings in their mouths – being excellent excretors of metals and not having any other significant, ongoing health challenges – there are some who can tolerate a root canal.
Now, this doesn’t mean that if you have root canals, you’re fated for cancer or other chronic disease. As we’ve noted before, the development of illness – and the type of illness that manifests – depends upon the health of your biological terrain. Just as there are some who can live for years with mercury fillings in their mouths – being excellent excretors of metals and not having any other significant, ongoing health challenges – there are some who can tolerate a root canal.
But because the risks are so very high, we don’t recommend the procedure. If a tooth truly is beyond saving, then you need to look at extraction and replacement with a biocompatible partial. Yes, even single tooth partials are an option with the latest light-weight, flexible materials, such as Valplast.
The best way to avoid root canals? Take good care of your teeth and gums now.